
CAMH News & Stories
In the headlines or behind the scenes, CAMH stories always aim to inform, engage, and enlighten.
- Home
- CAMH News & Stories

CAMH develops first ever clinically validated natural supplement to prevent postpartum blues
Product now available in the U.S. with global distribution planned
About CAMH develops first ever clinically validated natural supplement to prevent postpartum blues
CAMH forms strategic partnership to advance women's health
Supported by Manulife, a new alliance between womenmind™ and the Women’s Health Research Cluster helps advance gender parity in research
About CAMH forms strategic partnership to advance women's health
Breaking ground on a brighter future for mental health
New buildings will inspire hope and transform mental health care and research
About Breaking ground on a brighter future for mental health
CAMH’s STOP Program receives $850,000 from Ontario Ministry of Health
Funding will support new smoking and vaping cessation initiatives
About CAMH’s STOP Program receives $850,000 from Ontario Ministry of Health
CAMH and YouTube Health Partner to Promote Mental Health Literacy in Canada
In an effort to provide accessible, accurate, and high-quality health information to Canadians, YouTube and the Centre for Addiction and Mental Health (CAMH) are partnering as part of the global YouTube Health initiative.
About CAMH and YouTube Health Partner to Promote Mental Health Literacy in Canada
Our final phase of redevelopment: Discovery and Recovery
2024 kicks off the fourth and final stage of our historic redevelopment.
About Our final phase of redevelopment: Discovery and Recovery
CAMH Tops list of Mental Health Research Hospital Rankings
During the 2021-22 fiscal year, CAMH reached $86.6 million in research spending, a new record high and an 8.7 per cent increase over the prior year
About CAMH Tops list of Mental Health Research Hospital Rankings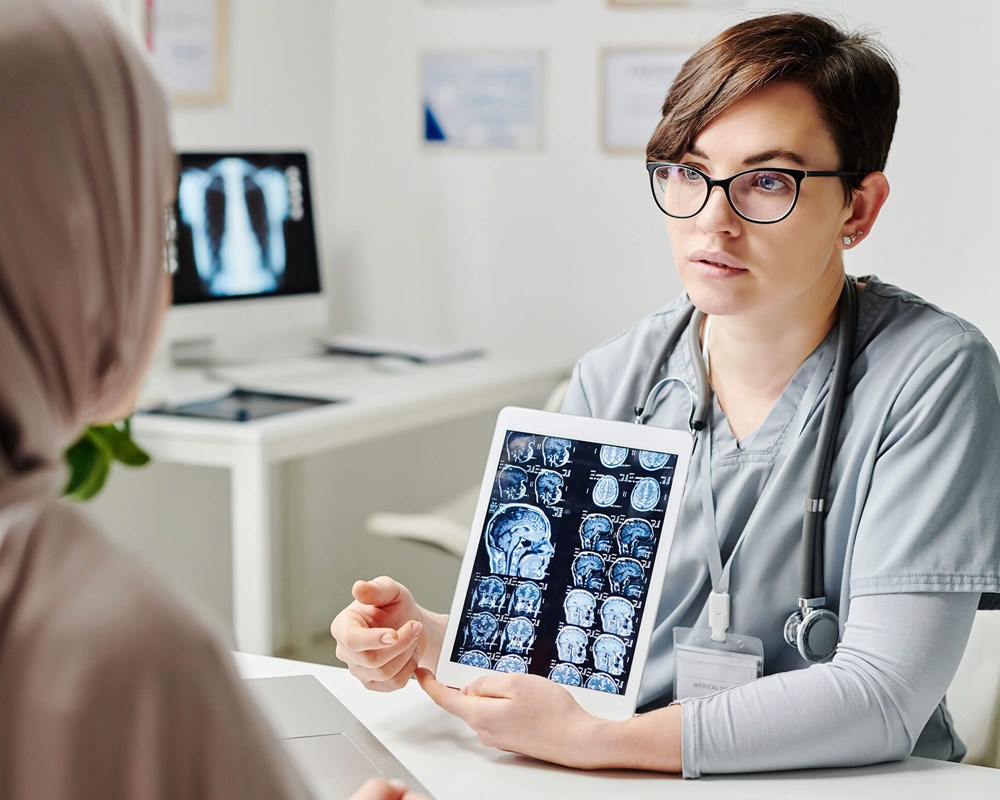
Open Science momentum grows stronger in Canada with a new commitment by its largest mental health teaching hospital
CAMH joins the Tanenbaum Open Science Institute alliance in a partnership to open research practices.
About Open Science momentum grows stronger in Canada with a new commitment by its largest mental health teaching hospital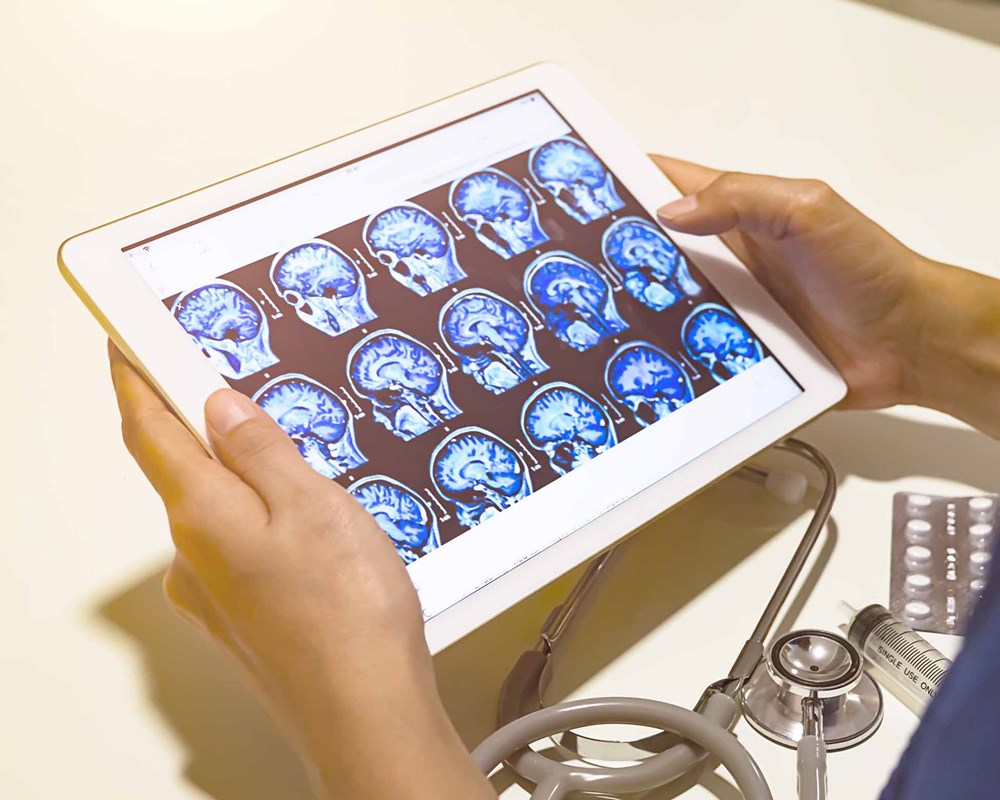
CAMH develops potential new drug treatment for multiple sclerosis
A small molecule drug that aids in the neuroprotection of cells found to be effective in treating nerve damage and symptoms in models of MS
About CAMH develops potential new drug treatment for multiple sclerosis
Canada’s 9-8-8: Suicide Crisis Helpline launches today
New three-digit suicide prevention helpline will take calls and texts, 24/7 anywhere in Canada
About Canada’s 9-8-8: Suicide Crisis Helpline launches today

